Three factors that impact caring for older adults in the United States today are occurring simultaneously. Together the factors make a compelling case for cancer providers to better support the needs of older adults and caregivers:
- Demography: The number of adults over the age of 65 is projected to double over the next 25 years.
- Complexity: Approximately 80 percent of older adults have at least one chronic disease, and 77 percent have at least two. Many of our health systems are ill-equipped to deal with the social complexity many older adults face.
- Disproportionate Harm: Older adults have higher rates of health care utilization as compared to other age groups and experience higher rates of health care-related harm, delay, and discoordination. One consequence of this is a rate of ED utilization that is four times that of younger populations.
Becoming an Age-Friendly Health System entails reliably providing a set of specific, evidence-based geriatric best practice interventions to all older adults in your health system. This is achieved primarily through redeploying existing health system resources to achieve:
- Better health outcomes for this population;
- Reduced waste associated with low-quality services;
- Increased utilization of cost-effective services for older adults; and
- Improved reputation and market share with a rapidly growing population of older adults.
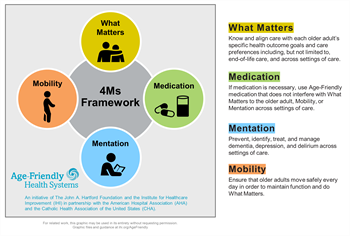
The 4Ms Framework of Age-Friendly Care
The 4Ms — What Matters, Medication, Mentation, and Mobility — make care of older adults that can be complex, more manageable. The 4Ms identify the core issues that should drive all care and decision making with the care of older adults. They organize care and focus on the older adult’s wellness and strengths rather than solely on disease. The 4Ms are relevant regardless of an older adult’s individual disease(s). They apply regardless of the number of functional problems an older adult may have, or that person’s cultural, ethnic, or religious background.
The 4Ms are a framework, not a program, to guide all care of older adults wherever and whenever they touch your cancer program’s care and services. The intention is to incorporate the 4Ms into existing care, rather than layering them on top, to organize the efficient delivery of effective care.
In 2020, the COVID-19 pandemic has put an increased burden on older adults, families, and staff in health systems. Perhaps especially during this challenging time, we have found that the 4Ms can reduce burden on care teams by providing an organizing framework to focus on the most critical care for older adults.
Age-Friendly Health Systems practice the 4Ms in every interaction with older adults. IHI recognizes care locations, such as hospitals, practices, retail-clinics, and nursing homes as Age-Friendly when they share a description of how they assess, document, and act on each of the 4Ms.
Download this one-pager to learn more and share with your colleagues.
Related Resources